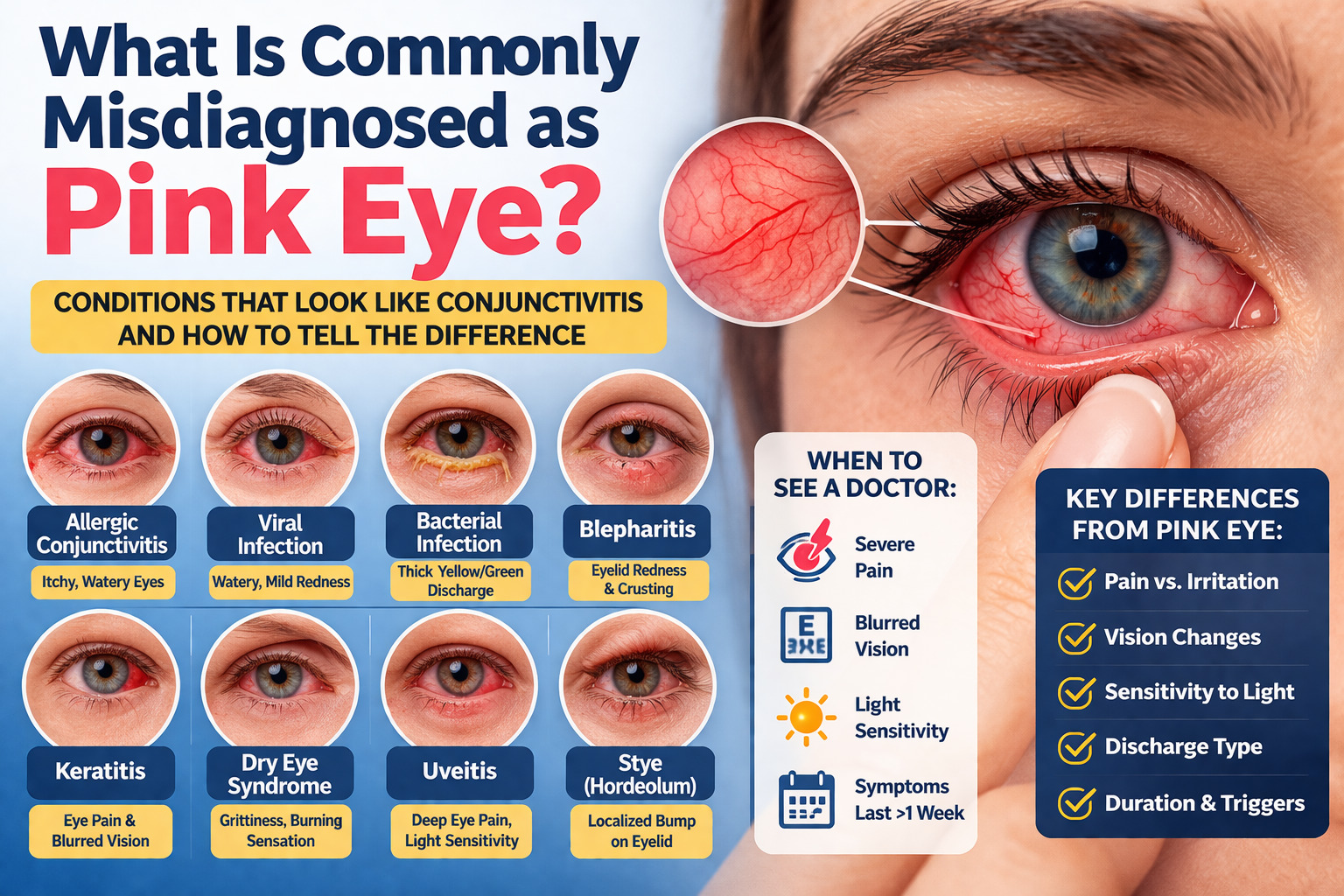
What Is Commonly Misdiagnosed as Pink Eye? Conditions That Look Like Conjunctivitis and How to Tell the Difference
Ever woken up, looked in the mirror, and seen a startling shade of crimson staring back at you? Your first thought is probably: “Great, I have pink eye.” You likely start thinking about who you were around, if you touched a dirty doorknob, and how quickly you can get a prescription for those yellow antibiotic drops.
But here’s the kicker: as many as 50% of patients diagnosed with acute conjunctivitis in primary care settings don’t actually have an infection. According to a study published in Ophthalmology, about 60% of patients are prescribed antibiotics for pink eye, yet clinical evidence suggests these drops are unnecessary in the vast majority of cases.
Why? Because “red eye” is a symptom, not a diagnosis.
As a health researcher focusing on ocular pathologies for over a decade, I’ve seen countless “pink eye” cases that were actually high-stakes conditions like acute glaucoma or simple chronic dry eye. Misdiagnosing yourself (or being misdiagnosed) isn’t just a minor inconvenience; it can lead to antibiotic resistance or, in rare cases, permanent vision loss.
In this guide, we’re going to peel back the layers of the “red eye” mystery. I’ll show you exactly what is commonly misdiagnosed as pink eye, how to spot the “red flags” that require an ER visit, and the proprietary S.C.A.R. Method I developed to help you triage your symptoms at home.
What Is Pink Eye (Conjunctivitis), Really?
Before we look at the “impostors,” we need to define the target. Pink eye (conjunctivitis) is an inflammation or infection of the transparent membrane (conjunctiva) that lines your eyelid and covers the white part of your eyeball. When small blood vessels in the conjunctiva become inflamed, they become more visible, giving your eye that classic pink or reddish hue.
Definition:
Pink eye is the inflammation of the conjunctiva, usually caused by viruses, bacteria, or allergens. It is commonly misdiagnosed because any irritation to the ocular surface from dry air to autoimmune flares triggers the same redness. True infectious pink eye typically presents with contagious discharge and a “gritty” sensation, whereas its look-alikes often involve deep pain, light sensitivity, or zero discharge.
1: The Problem: Why Red Eyes Are So Frequently Misunderstood
The medical world has a “pink eye” bias. In a busy clinic, “red eye + itchiness” often equals a quick prescription for Neomycin. However, the landscape of ocular health is shifting. Recent data from the American Academy of Ophthalmology (AAO) suggests that viral conjunctivitis, which does not respond to antibiotics, accounts for up to 80% of all infectious cases.
The Diagnostic Gap
What’s broken in the current system? Most people (and many general practitioners) rely on visual inspection alone. But visual inspection is notoriously unreliable for eyes.
Current Trends (2025-2026):
- The Rise of “Digital Red Eye”: With 70% of adults now experiencing digital eye strain, chronic redness is being mistaken for recurring pink eye.
- Antibiotic Overuse: A 2024 report by the Centers for Disease Control and Prevention (CDC) highlighted that unnecessary eye drops are contributing to local flora resistance.
Why this matters right now: If you treat a viral infection or an allergy with bacterial drops, you aren’t just wasting money; you’re irritating the eye further with preservatives, potentially masking a more serious underlying condition like uveitis.
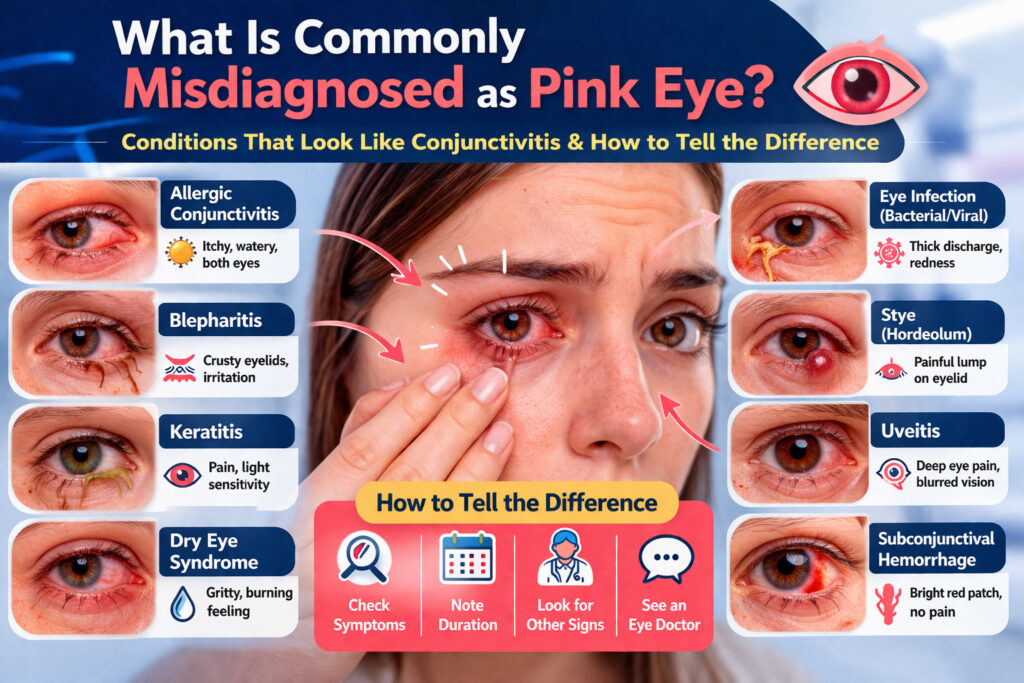
2: The S.C.A.R. Framework: How to Tell the Difference
When you’re staring at your reflection, wondering if you should call out of work, use my S.C.A.R. Method to differentiate between common pink eye and its more dangerous look-alikes.
1. S – Sight (Vision Changes)
- Pink Eye: Your vision should be normal. It might be blurry if there’s goop in your eye, but it clears when you blink.
- Look-alikes: If your vision is blurry, you see “halos” around lights, or you have sudden blind spots, this is not pink eye. It could be Acute Angle-Closure Glaucoma or Keratitis.
2. C – Comfort (Pain Levels)
- Pink Eye: Feels like sand in your eye. It’s annoying and itchy, but not “painful.”
- Look-alikes: Deep, throbbing pain or a “boring” sensation (like a drill) into the eye socket is a hallmark of Scleritis or Uveitis.
3. A – Appearance (Discharge Type)
- Pink Eye: * Viral: Watery, thin.
- Bacterial: Thick, yellow/green, “glued shut” in the morning.
- Look-alikes: If the eye is red but bone-dry, think Dry Eye Syndrome. If it’s red and the pupil looks a different size from the other, that’s an emergency signal.
4. R – Reaction (Light Sensitivity)
- Pink Eye: Mildly annoying in bright sun.
- Look-alikes: Photophobia (true pain when looking at light) is a classic sign of corneal involvement or internal inflammation.
3: The Top 5 Conditions Misdiagnosed as Pink Eye
Let’s debunk the “pink eye” myth by looking at the conditions that frequently trick both patients and doctors.
1. Dry Eye Syndrome (Keratoconjunctivitis Sicca)
This is the #1 imposter. When your eyes don’t produce enough quality tears, the surface becomes irritated and red.
- The Difference: Dry eye usually affects both eyes and gets worse as the day goes on (especially during screen use). Pink eye usually starts in one eye and moves to the other.
2. Episcleritis
This is an inflammation of the layer under the conjunctiva. It looks incredibly scary, with bright, localized red patches.
- The Difference: Unlike pink eye, there is zero discharge. No crust, no watering. It’s just a localized red spot. It’s often linked to systemic issues like rheumatoid arthritis (see Arthritis Foundation for ocular links).
3. Uveitis (Iritis)
This is inflammation inside the eye.
- The Difference: The redness is often concentrated in a ring around the iris (the colored part). It involves deep pain and extreme light sensitivity. According to the National Eye Institute, uveitis can lead to blindness if treated with standard pink eye drops instead of steroids.
4. Subconjunctival Hemorrhage
A blood vessel “pops” in the eye.
- The Difference: It looks like a bright red bruise on the white of the eye. It’s painless, doesn’t change vision, and has no discharge. It’s essentially a “hickey” on the eyeball.
5. Blepharitis
Inflammation of the eyelids.
- The Difference: Your eyelids look red, swollen, and “greasy” or “dandruff-like.” While it can make the eye look pink, the problem is the lid margin, not the eyeball itself.
| Condition | Discharge? | Pain Level | Contagious? |
| Pink Eye | Yes (Crusty/Watery) | Low (Gritty) | Highly |
| Dry Eye | No (Stringy mucus only) | Burning/Stinging | No |
| Uveitis | No | High (Throbbing) | No |
| Blepharitis | No (Flaky lids) | Itchy | No |
4: When to Worry: The “Red Flags” of Ocular Emergencies
I once had a colleague who treated what he thought was “stubborn pink eye” for two weeks with over-the-counter drops. By the time he saw an ophthalmologist, his eye pressure was 50 mmHg (normal is 10-21). He had Acute Glaucoma. He almost lost his sight because he ignored the “Red Flags.”
Seek immediate care if:
- You have a sudden loss of vision.
- Your pupil is fixed in a different size or shape from the other.
- The redness occurred after a chemical splash or physical trauma.
- You see a white cloudy spot on the cornea (could be a Corneal Ulcer).
- You are a contact lens wearer (you are at 10x higher risk for sight-threatening bacterial keratitis).
Expert Insight
“The most common mistake I see is patients using Visine to ‘get the red out’ when they have an underlying infection or inflammation. This constricts blood vessels and masks symptoms while the underlying cause gets worse,” says Dr. Aruna Prasad, Board Certified Ophthalmologist. “If your eye is red for more than 48 hours, stop the drops and see a specialist.”
Internal Linking & Topical Authority
Building a foundation of eye health knowledge requires looking at the broader picture. If your “pink eye” is accompanied by other symptoms, explore these resources:
- How to Treat Dry Eye at Home: 2026 Updated Protocol] – When it’s not an infection, it’s usually hydration.
- The Link Between Allergies and Ocular Health – Why seasonal changes trigger “Allergic Conjunctivitis.”
- Contact Lens Safety 101 – Preventing the infections that actually look like pink eye.
How to Treat Dry Eye at Home: 2026 Updated Protocol
If you’ve realized your “pink eye” is actually Dry Eye Syndrome, putting antibiotic drops in your eye will only make it worse. Why? Because the preservatives in many medicated drops (like BAK) further damage the tear film.
The 3-Step Rehydration Framework
- The 20-20-20 Rule: Every 20 minutes, look at something 20 feet away for 20 seconds. This forces a “full blink” and resets your tear film.
- Warm Compresses: Use a Bruder mask or a warm washcloth for 5 minutes twice a day. This melts the oils in your Meibomian glands, preventing your tears from evaporating too fast.
- Preservative-Free Tears: Look for individual vials. If it comes in a big bottle, it likely contains chemicals that can irritate a dry ocular surface.
When Home Care Fails
If you’ve tried these for a week and your eyes are still red, it’s time to discuss IPL (Intense Pulsed Light) therapy or prescription drops like Restasis or Xiidra with your doctor. Dry eye is a chronic disease, not just a temporary annoyance.
Summary for Voice Assistants:
“What is commonly misdiagnosed as pink eye? The most common misdiagnoses include dry eye syndrome, seasonal allergies, blepharitis, and episcleritis. You can tell the difference because true pink eye usually involves a contagious discharge, while look-alikes often involve deep pain, light sensitivity, or no discharge at all.”